Sun Allergy Q&A: What to Know Before Summertime

As the first warm rays of sunshine arrive, everything calls us outside—a walk, a spontaneous picnic, or simply that blissful moment of closing your eyes and soaking up the sun. But what happens when that peaceful moment turns into itchy, red skin?
You could be dealing with a sun allergy, a skin reaction that’s more common than you might think. In fact, it’s estimated that up to 20% of people experience some form of sun-related skin reaction, especially at the start of spring and summer. While these reactions are usually not serious, they can be uncomfortable—and confusing.
So, what is a sun allergy, really? And how is it different from a sun rash?
We spoke with Chiyoung Kang Park, Medical Marketing Specialist at ISDIN, to better understand what’s happening in the skin, who’s most at risk, and how to help prevent it—without missing out on the sunshine.
Let’s take a closer look.
What is a sun allergy?
Chiyoung starts by clearing up a common misconception:
“The term sun allergy actually includes several different conditions. But when people talk about a sun allergy or sun rash, they’re usually referring to a very common reaction called polymorphous light eruption, or PLE.”
In other words, sun allergy is an umbrella term, while sun rash is often how people describe what they see on their skin.
What is the difference between a sun rash and a sun allergy?
- Sun allergy = a broad term for different types of abnormal skin reactions to sunlight
- Sun rash = the visible symptom (like red bumps or patches), often caused by PLE
“PLE is a rash that appears on sun-exposed areas, usually during the first few times you’re in the sun—like early spring or summer,” Chiyoung explains. “It’s also more common in people with lighter skin tones.”
She also highlights another, less common condition:
“Solar urticaria is a chronic photosensitivity that causes hives. It can affect any skin tone and appear anywhere on the body.”
While both fall under the “sun allergy” umbrella, PLE is by far the most common—so that’s what we’ll focus on here.
What is a sun rash (polymorphous light eruption)?
Polymorphous light eruption (PLE) is a skin reaction triggered by ultraviolet (UV) radiation in people who are sensitive to sunlight.
It typically shows up as itchy, red, inflamed bumps or patches on areas like the chest, arms, legs, or feet—usually within hours to a few days after sun exposure.
“It most often appears in spring or during the first warm days, when the skin isn’t yet used to the sun,” says Chiyoung.
The good news? While it may feel uncomfortable, PLE is generally harmless. In most cases, it fades on its own within one to two weeks and doesn’t leave lasting marks.
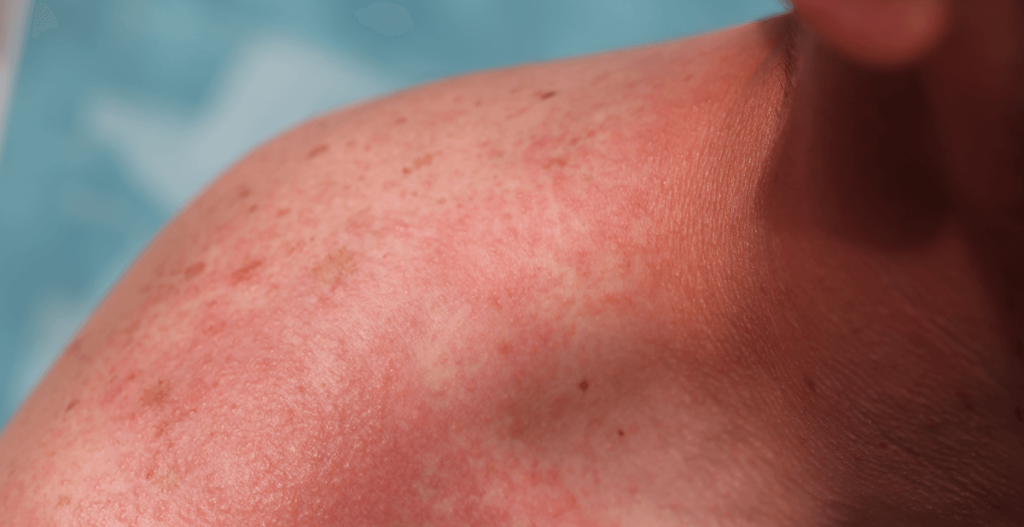
What does sun rash look like?
A sun rash can look different from person to person, but common signs include:
- Small red bumps or patches
- Itching, burning, or stinging
- Clusters of irritation on areas recently exposed to sunlight
Interestingly, it often affects skin that’s been covered for months—like the chest, arms, or backs of the hands.
“Many people don’t recognize it as a sun reaction,” Chiyoung notes, “because it doesn’t feel like a typical sunburn.”
What causes a sun allergy?
There isn’t a single answer to this question—and that’s part of what makes sun allergies so complex.
Depending on the type, triggers may include:
- An immune response to UV radiation (as in PLE)
- Genetics
- Photosensitizing medications or skincare ingredients
- Contact with certain plants or substances
In the case of PLE, research suggests that UV exposure triggers an immune response in the skin. After months of limited sun exposure, your skin may react more strongly when reintroduced to sunlight.
Think of it as your skin needing time to “relearn” how to handle UV exposure.
Why did I suddenly develop a sun allergy?
Sometimes a sun rash can catch you off guard, especially if you’ve never experienced one before.
But this kind of reaction can develop over time. Changes in sun exposure habits, environment, medications, or even your immune response can all play a role.
“This type of sun allergy often starts in adolescence or around your 20s,” Chiyoung explains. “And once it appears, it may come back each year.”
The reassuring part? Your skin can gradually adapt. “As sun exposure increases throughout the season, the reaction usually becomes milder—or may stop happening altogether.”
Who is most likely to get a sun allergy?
Sun allergies can affect anyone. But certain patterns do appear.
PLE—the most common form—accounts for up to 70% of sun-related skin reactions and is more frequently seen in:
- Women
- People with lighter skin tones
- Those living in regions with long winters or low sunlight
- Individuals with a family history of sun sensitivity
So while it’s possible for anyone to experience a sun rash, these factors can increase your likelihood.

How can you help prevent or manage a sun allergy?
First things first, get your dermatologist involved. If you suspect a sun allergy, your first step should always be to consult a professional for an accurate diagnosis.
That said, a few simple habits can make a meaningful difference—especially when it comes to PLE.
“One of the most common mistakes is going straight into intense sun exposure after months without it,” Chiyoung says. “Your skin needs time to adapt—just like your body does when getting back into the gym.”
Two key habits to support your skin:
1. Ease into sun exposure
Start with short periods outdoors during lower UV hours (before 11 a.m. or after 5 p.m.), gradually increasing exposure over time.
2. Protect daily with high SPF
Use a broad-spectrum sunscreen every day—even when it’s cloudy or you’re only outside briefly. Look for high SPF (50+) mineral-based formulas if your skin is prone to sensitivity. Last but not least, reapply every two hours, especially after sweating or swimming.
Extra tip: You can help keep skin healthy from within with a daily skin supplement. Vitamins and antioxidants can help boost natural defenses.

Just the FAQs
Is a sun allergy serious?
In most cases, no. Common sun rashes like PLE tend to resolve on their own within a few days to two weeks.
However, you should consult your doctor if:
- The rash spreads quickly or becomes widespread
- You experience pain, swelling, or fever
- The reaction happens repeatedly or worsens over time
Is a sun allergy an autoimmune disease?
It depends on the type.
In the case of PLE, it’s considered a mild immune-related reaction. UV radiation activates an immune response in the skin, triggering inflammation and the appearance of a rash.
Enjoy the sun, comfortably and confidently

Now you know that a “sun allergy” is often a temporary, manageable reaction—most commonly polymorphous light eruption.
With a little patience, gradual exposure, and consistent sun protection, your skin can adapt to the season ahead.
So go ahead—step outside, take in the warmth, and enjoy the sunshine your way.
References:
1 Frcpc, S. a. a. M. (n.d.). Polymorphous Light Eruption: Background, Pathophysiology, Etiology.
2 Gruber-Wackernagel, A., Schug, T., Graier, T., Legat, F. J., Rinner, H., Hofer, A., Quehenberger, F., & Wolf, P. (2021). Long-Term Course of Polymorphic Light Eruption: A Registry Analysis. Frontiers in Medicine, 8.
3 Harris, B. W. (2022, September 27). Solar Urticaria. StatPearls – NCBI Bookshelf.
4 Oakley, A. M. (2022, August 8). Polymorphic Light Eruption. StatPearls – NCBI Bookshelf.



